

This study evaluates how steam autoclave sterilization at different temperatures affects the mechanical performance of 3D-printed surgical guides made with Custom Guide Resin (Custom Resin Solutions, Antalya, Türkiye). The primary outcomes were flexural modulus and flexural strength, measured by a three-point bending test. The study also compares guide accuracy before and after sterilization at 121°C (>1 bar, 20 min) and 134°C (>2 bar, 10 min) to identify an optimal sterilization protocol that maintains clinical performance.
Implant-supported restorations have become increasingly common in modern dentistry due to their accuracy and predictable clinical outcomes. Multiple studies report high long-term success and survival rates for implant-supported treatments. During guided implant surgery, surgical guides can contact tissues, blood, and mucous membranes. If guides are not properly sterilized, microorganisms may enter the surgical site and compromise healing, treatment success, and implant lifespan.
Sterilization is defined as the complete elimination of all forms of microbial life using physical or chemical processes, while disinfection reduces microorganisms and may not reliably eliminate bacterial spores. According to CDC guidance, devices that contact blood and tissues are considered higher-risk and typically require high-level sterilization. In dental practice, steam autoclave sterilization remains widely used due to its practicality, cost-effectiveness, and established sterilization performance.
Eighteen standardized specimens were produced using an LCD-based 3D printer (PioCreat C-01, PioCreat 3D, Shenzhen, China) with a 50 µm layer thickness. Specimens were printed with Custom Guide Resin (Custom Resin Solutions, Antalya, Türkiye). After cleaning with isopropyl alcohol, all specimens were post-cured using a nitrogen-inert environment with an Otoflash G17 device (NK Optik, Baierbrunn, Germany), applying 2000 flashes (1000 flashes per side).
Specimens were divided into three groups (n = 6 per group):
Mechanical testing was performed using a three-point bending test on a Zwick Z250 universal testing machine (ZwickRoell, Yokohama, Japan). The crosshead speed was 5 mm/min, and results are reported as mean values for each group.
To visualize the impact of sterilization conditions on material behavior, results are presented in graphical and tabular formats. The figures below show flexural modulus and flexural strength changes across the three groups, enabling a direct comparison of performance before and after autoclave sterilization.
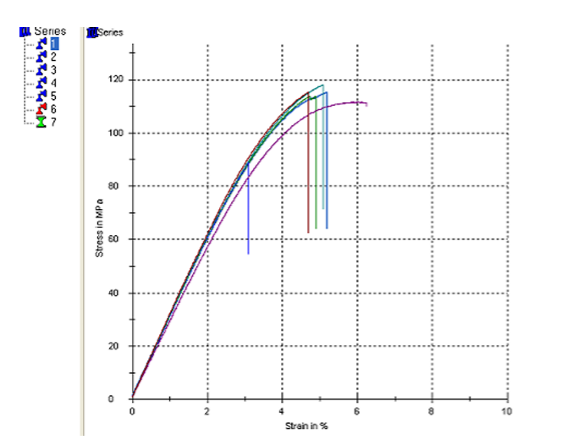
Figure 1: Three-point bending test results for Group A (Control)
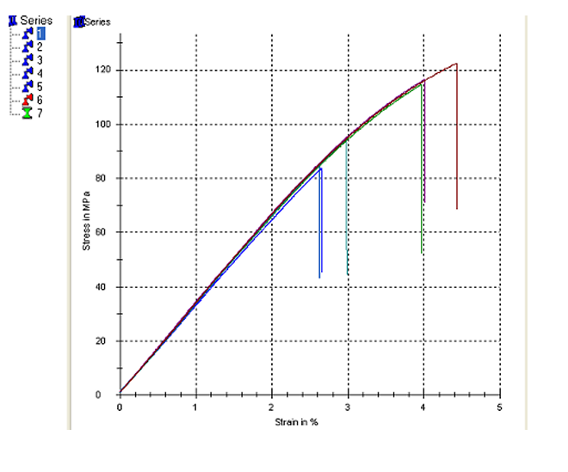
Figure 2: Three-point bending test results for Group B (121°C)
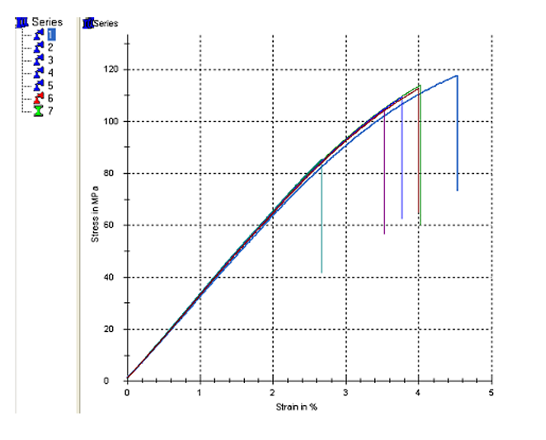
Figure 3: Three-point bending test results for Group C (134°C)
| Group | Flexural Modulus (MPa) | Flexural Strength (MPa) |
|---|---|---|
| A (Control) | 3001 | 110.4 |
| B (121°C) | 3272 | 102.7 |
| C (134°C) | 3216 | 107.2 |
Table 1: Mean flexural modulus and flexural strength values for each group (n = 6)
Steam autoclave sterilization at 121°C and 134°C produced only minor changes in the flexural modulus and flexural strength of 3D-printed specimens made with Custom Guide Resin. Flexural modulus showed an increase after sterilization, but the change was not statistically significant, suggesting that autoclaving does not adversely affect stiffness.
A small reduction in flexural strength was observed after sterilization; however, values remained within clinically acceptable limits. The decrease was less pronounced at 134°C, suggesting that the 134°C protocol may be preferable when prioritizing mechanical stability. Importantly, differences between the two sterilization protocols were limited, indicating that both can be used confidently in clinical practice.
Overall, these findings support that Custom Guide Resin maintains mechanical integrity after autoclave sterilization and remains a reliable material choice for guided implant surgery where sterile workflow and mechanical performance are essential.
Learn more about our dental 3D printing resin solutions designed for accuracy, safety, and regulatory compliance.
#SurgicalGuideResin #DentalSurgicalGuide #GuidedImplantSurgery #ImplantDentistry #DentalImplants #DigitalDentistry #Dental3DPrinting #Dental3DPrintedGuides #3DPrintedSurgicalGuide #AutoclaveSterilization #SteamSterilization #DentalSterilization #MedicalDeviceSterilization #InfectionControl #CDCGuidelines #ISO11139 #FlexuralStrength #FlexuralModulus #ThreePointBendingTest #DentalMaterials #BiocompatibleResin #CustomGuideResin #CustomResinSolutions